Cervical Spine Surgery: Types and Considerations
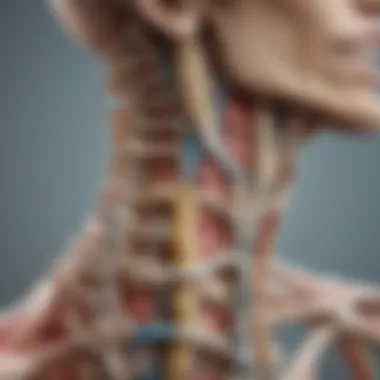

Intro
Cervical spine surgery addresses vital health issues relating to the neck and upper spine. This field includes a variety of surgical techniques aimed at treating conditions such as herniated discs, spinal stenosis, and trauma. Each surgical approach holds its unique indications and methodologies and understanding these is important for both patients and medical professionals. This article seeks to provide a comprehensive overview of cervical spine surgeries, reflecting on their complexities, applications, and implications.
Various types of surgeries exist, and each serves distinct purposes. By categorizing these procedures, this text offers clarity and insight into how they can influence recovery and overall spinal health. The importance of tailoring these options to meet individual patient needs cannot be understated. It forms the crux of effective healthcare within this field.
Key Findings
Cervical spine surgery represents a crucial component of musculoskeletal medicine. The most significant findings from recent research and clinical practices reveal several key points:
- Diverse Surgical Types: Procedures such as anterior cervical discectomy and fusion (ACDF), cervical fusion, and cervical laminectomy address various spinal disorders.
- Personalized Treatment Plans: Individualized approaches optimize outcomes, as surgeries depend greatly on the specific condition and patient needs.
- Advanced Techniques: Advancements in minimally invasive techniques reduce recovery times and associated risks.
The significance of these findings extends beyond individual surgeries. They underscore a shift towards more tailored approaches in treatment, increasingly prevalent in surgical procedures. This evolution benefits both practitioners and patients, enhancing surgical outcomes and satisfaction.
"Understanding the nuances of cervical surgeries is pivotal for making informed decisions that align with patient needs and expectations."
Serving a broad spectrum of individuals, these surgical options offer not just solutions for pain but also restoration of function, affecting daily life significantly.
Implications of the Research
The implications of various surgical findings influence numerous real-world applications:
- Clinical Practices: Enhanced knowledge guides practitioners in selecting the appropriate procedure based on specific diagnoses.
- Patient Education: Informing patients about surgical options increases their involvement in the treatment process, promoting better health decisions.
Potential future research directions might focus on long-term outcomes associated with different surgical techniques. Continued exploration of technologies and methodologies could lead to improved techniques and recovery outcomes in cervical spine surgeries.
As the field continues to develop, understanding these implications remains crucial for ongoing advancements in cervical spine surgery. This highlights a commitment to not only treat but also innovate in patient care.
Intro to Cervical Spine Surgery
Cervical spine surgery represents a critical intervention for treating disorders affecting the neck and the upper spine. Understanding the nuances of this type of surgery is vital, as it encompasses various techniques, indications, and potential outcomes. In this article, readers will explore significant concepts regarding cervical spine surgery, which can serve as a guide for patients and healthcare professionals alike. The importance of this overview lies in its potential to illuminate the often complex choices that face individuals suffering from spinal ailments.
Overview of Cervical Spine Anatomy
The cervical spine consists of seven vertebrae, labeled C1 to C7. These vertebrae protect the spinal cord, support the head, and facilitate a wide range of neck movements. Each vertebra is separated by intervertebral discs that aid in cushioning the spine and allowing flexibility. The anatomy is not only vital for understanding the function of the cervical spine but is also significant when considering surgical interventions. Surgeons must have a thorough understanding of the anatomy to effectively address issues such as herniated discs, spinal stenosis, and degenerative diseases.
Disorders like cervical radiculopathy or myelopathy can arise from various factors, including degenerative changes or trauma. The interplay between these structures is complex; therefore, a detailed knowledge of cervical anatomy is essential. It equips medical professionals to identify problem areas accurately and choose the most effective surgical approach.
Common Indications for Surgery
Several conditions may necessitate cervical spine surgery. Common indications include:
- Herniated Discs: Discs can bulge or rupture, pressing on spinal nerves and causing pain or neurological symptoms.
- Cervical Stenosis: Narrowing of the spinal canal can lead to pressure on the spinal cord and nerves, resulting in severe pain and limited mobility.
- Degenerative Disc Disease: Over time, discs can weaken, leading to chronic pain and instability.
- Trauma or Fractures: Injuries to the cervical spine may require surgical intervention to stabilize the area and prevent further damage.
Identifying the right timing and necessity for surgery is crucial. Not all conditions require surgical treatment; some may be managed effectively with conservative methods such as physical therapy or medication. However, when conservative treatments fail, surgery may offer substantial relief and improved quality of life.
Understanding cervical spine surgery encompasses acknowledging when such interventions are required and their importance in restoring function and alleviating pain. This knowledge can guide patients toward appropriate treatment and ensure they make informed decisions alongside their healthcare providers.
Types of Cervical Spine Surgery
Cervical spine surgery is a significant field within neurosurgery and orthopedics. It addresses various pathologies affecting the cervical vertebrae, intervertebral discs, and spinal cord. The importance of understanding the types of cervical spine surgeries lies in their distinct indications, techniques, and potential outcomes. This section aims to clarify the different surgical options and help patients and healthcare providers make informed choices.
Anterior Cervical Discectomy and Fusion (ACDF)
Anterior Cervical Discectomy and Fusion (ACDF) is a widely performed procedure. It involves removing a herniated or degenerative disc, followed by the fusion of adjacent vertebrae. This process aims to alleviate pressure on the spinal cord and nerves. The procedure is beneficial for patients suffering from cervical radiculopathy or myelopathy. The approach is through the front of the neck, providing direct access to the affected disc.
Benefits of ACDF:
- Reduction in pain and neurological symptoms
- Stabilization of the cervical spine
- High success rates for symptom relief
Considerations include the potential for adjacent segment disease. This occurs when the discs next to the fusion site undergo degeneration over time. Thus, it is essential for surgeons and patients to discuss long-term implications.
Posterior Cervical Foraminotomy
Posterior Cervical Foraminotomy is a less invasive option for relieving nerve root compression. It involves the removal of bone spurs or tissue pressing on neural structures, allowing for better space for the nerve roots. Patients with radiculopathy may find this procedure improves their quality of life.


Key Points to Note:
- Preserves disc integrity and motion
- Can often be performed as an outpatient procedure
- Minimal muscle dissection required
Such advantages make Posterior Cervical Foraminotomy ideal for tailored treatment plans, especially for patients seeking to retain motion in their spine.
Cervical Laminectomy
Cervical Laminectomy involves the removal of the lamina, a bony structure protecting the spinal cord. This procedure is generally considered for patients with spinal stenosis, where narrowing of the spinal canal occurs. The goal is to relieve pressure on the spinal cord, thereby reducing neurological deficits.
Important Considerations:
- Can lead to instability requiring further procedures
- Recovery may take longer
Despite these challenges, many patients experience significant relief from symptoms and improved function after this surgery.
Cervical Artificial Disc Replacement (ADR)
Cervical Artificial Disc Replacement is a newer option when compared to traditional fusion. In this procedure, a damaged disc is replaced with an artificial one, thereby preserving motion in the cervical spine. This is especially beneficial for younger patients or those with a single-level disc disease.
Benefits of ADR:
- maintains the natural motion of the spine
- potentially less adjacent segment degeneration
- Faster recovery compared to fusion options
However, long-term outcomes are still under investigation, and careful selection of candidates is crucial.
Cervical Stabilization and Fusion Techniques
Cervical Stabilization and Fusion Techniques encompass various approaches, typically used in more complex cases involving instability or multiple levels of degeneration. These techniques aim to stabilize the spine and promote bone growth between adjacent vertebrae.
Types of Stabilization Techniques:
- Plate and screw systems
- Cages combined with grafts
Effective stabilization minimizes the risk of future complications. Therefore, discussions about the best method should be thorough, considering individual patient needs and anatomy.
Each type of surgery entails specific benefits, considerations, and patient outcomes. Understanding these surgical options enhances not only the appreciation of their complexities but also aids informed decision-making between patients and healthcare providers.
Minimally Invasive Cervical Spine Surgery
Minimally invasive cervical spine surgery has gained prominence in the field of spinal surgery. This shift largely reflects advancements in surgical techniques and technology that aim to reduce patient recovery time and improve surgical outcomes. These procedures allow surgeons to access cervical structures without the need for extensive incisions. Instead of traditional large openings, small incisions and specialized tools are used. This approach mitigates trauma to surrounding tissues, leading to less postoperative discomfort and faster recovery.
The significance of minimally invasive techniques stems from various factors. Patients experience a quicker return to normal activities due to reduced soft tissue injury. Factors like diminished blood loss during surgery and a decreased length of hospital stay further emphasize its advantages. Moreover, the potential for lower complication rates attracts both patients and surgical teams toward these procedures. As spinal disorders become more prevalent, understanding the benefits of minimally invasive surgery is essential for making informed treatment decisions.
Advantages of Minimally Invasive Techniques
Several key advantages characterize minimally invasive cervical spine surgery. These include:
- Reduced Surgical Trauma: Smaller incisions lead to less muscle and tissue disruption. The body experiences less pain and swelling, which contributes to a smoother recovery.
- Shorter Hospital Stay: Many patients can leave the hospital within one to two days post-operation, compared to traditional methods that may require longer stays.
- Lower Risk of Infection: Smaller wounds reduce the surface area exposed to potential infections, which is crucial in surgical recovery.
- Quicker Recovery Time: Patients often return to their daily activities faster, which is beneficial for both personal and professional life.
- Enhanced Visualization: Techniques like endoscopic surgery allow surgeons to view the surgical site with great precision, leading to better outcomes.
This array of benefits highlights the importance of considering minimally invasive options when addressing cervical spine issues. The evolution toward these methods aligns with the goal of providing effective treatment while minimizing patient discomfort.
Common Minimally Invasive Procedures
Several common minimally invasive procedures are performed to treat various cervical conditions. Each procedure is tailored to specific patient needs and underlying conditions:
- Minimally Invasive Anterior Cervical Discectomy and Fusion (ACDF): A modified version of the traditional ACDF, this technique utilizes small incisions to remove herniated discs and fuse the vertebrae without extensive disruption of surrounding structures.
- Endoscopic Cervical Foraminotomy: This procedure helps alleviate nerve compression by removing bone spurs or other obstructions with the aid of an endoscope, minimizing injury to surrounding tissues.
- Cervical Laminectomy: Similar to the standard laminectomy but executed through small incisions, this technique relieves pressure on the spinal cord by removing part of the lamina.
- Robotic-Assisted Surgery: Utilizing advanced robotics, this method enhances precision in surgical tasks, potentially leading to better outcomes and reduced recovery time.
Understanding these procedures and their applications allows both patients and healthcare providers to make more informed decisions regarding treatment strategies. As minimally invasive techniques continue to advance, their role in cervical spine surgery is likely to expand, providing better care for patients with spinal disorders.
Surgical Techniques and Approaches
In the realm of cervical spine surgery, the choice of surgical technique significantly shapes patient outcomes. Techniques can broadly be classified as open surgery or endoscopic approaches. Each technique has unique characteristics, advantages, and considerations that influence the overall success of the intervention. Understanding these surgical methods is vital for practitioners and patients as they navigate treatment options. Factors like recovery time, potential for complications, and overall effectiveness are crucial elements in making informed decisions about surgery.
Open Surgery Techniques


Open surgery techniques involve larger incisions to provide surgeons with comprehensive access to the cervical spine. These procedures enable detailed visualization of the spine's anatomy, which can be beneficial during complex surgeries.
Generally, open surgery is preferred in cases where significant structural modifications or decompressions are necessary. For instance, Anterior Cervical Discectomy and Fusion (ACDF) often falls into this category, effectively addressing spinal nerve compression issues.
Key Benefits:
- Access: Maximal exposure allows for precise work on the spinal structures.
- Complex Cases: Suitable for complicated conditions or those requiring substantial intervention.
- Direct Visualization: Enhances the ability to see anatomical structures clearly, reducing the risk of error.
Considerations:
- Recovery Time: Typically, patients may experience longer recovery compared to minimally invasive options.
- Infection Risk: Due to larger incisions, there is an elevated risk of post-operative infections.
- Pain Management: Patients may require more extensive pain management solutions post-surgery.
Endoscopic Approaches
Endoscopic approaches represent a shift toward less invasive surgical techniques, often utilizing smaller incisions and specialized instruments. These methods are designed to minimize soft tissue disruption, aiming for quicker recovery times. With advancements in technology, endoscopic surgery has become an essential option for many cervical spine conditions.
One of the most common endoscopic procedures is the posterior cervical foraminotomy, which addresses nerve root compression with a less invasive strategy.
Key Benefits:
- Minimal Tissue Damage: Less trauma to surrounding tissues facilitates quicker healing.
- Shorter Hospital Stay: Many patients may be released the same day as surgery.
- Reduced Scarring: Smaller incisions lead to less visible scarring.
Considerations:
- Technology Dependent: Requires advanced technology and skilled surgeons comfortable with endoscopic techniques.
- Not Suitable for All Conditions: There are specific conditions where open surgery may still be the preferred option due to complexity.
- Learning Curve: Surgeons may need additional training to become proficient in these techniques.
"Choosing the right surgical approach is crucial for optimizing outcomes in cervical spine procedures. The decision often depends on patient-specific factors and the nature of their spinal condition."
Risks and Considerations in Cervical Spine Surgery
Understanding the risks and considerations associated with cervical spine surgery is crucial. This section highlights the importance of recognizing potential complications and factors that can influence surgical outcomes. Knowledge of these elements is imperative for both patients and healthcare providers, as it allows for better-informed decisions and expectations surrounding surgical interventions.
Potential Complications
Cervical spine surgery, like any surgical procedure, carries inherent risks. Potential complications can range from minor to severe. Key complications may include:
- Infection: Infection at the surgical site can occur, possibly leading to increased recovery time or the need for further interventions.
- Nerve Damage: Surgical manipulation near nerve roots may inadvertently cause damage, potentially resulting in numbness, weakness, or other neurological deficits.
- Blood Clots: Post-surgical patients may face a risk of blood clots, which can result in serious complications if not addressed promptly.
- Hardware Failure: In surgeries that involve implants, such as fusion procedures, there is a risk of implants failing or breaking over time, necessitating additional surgery.
- Cerebrospinal Fluid Leak: This can happen during surgical procedures, leading to headaches and other issues that may require further intervention.
"Acknowledging these complications helps in outlining a comprehensive care plan both before and after surgery, allowing for a more tailored approach to each patient’s needs."
Patients and surgeons must engage in thorough discussions to assess these risks. Establishing a comprehensive pre-operative evaluation is critical in identifying patient-specific factors that may exacerbate risks.
Factors Influencing Surgical Outcomes
Several variables impact the surgical outcomes of cervical spine procedures. Recognizing these factors can guide better expectations and outcomes. The following elements should be taken into account:
- Patient Health Status: Comorbidities such as diabetes and hypertension can adversely affect healing and lead to complications.
- Age: Older patients might have slower recovery times and a higher risk of complications, influencing overall outcomes.
- Lifestyle Factors: Smoking and obesity are known to negatively impact surgical outcomes. Smoking reduces blood flow, impeding healing, while obesity may complicate surgery itself and extend recovery.
- Surgeon Experience: The surgeon's expertise and familiarity with specific procedures are vital in minimizing complications and optimizing outcomes.
- Postoperative Care: Adequate follow-up and rehabilitation play a pivotal role in recovery. Engaging in recommended therapy and adhering to medical advice are crucial for successful outcomes.
Each of these factors underscores the importance of individualized treatment plans. Surgery is not merely a procedure but part of a broader continuum of care that includes pre-operative assessments and postoperative rehabilitation.
Postoperative Care and Rehabilitation
Postoperative care and rehabilitation play a vital role in the success of cervical spine surgery. The journey does not end once the surgery is completed; rather, it marks the beginning of a phase focused on recovery and the attainment of optimal functional outcomes. Effective management during this period can greatly influence overall healing, pain management, and the eventual return to normal activities.
Key elements of postoperative care include monitoring vital signs, managing pain levels, and preventing complications such as infection or blood clots. Specific benefits of structured rehabilitation following surgery are substantial. They range from restoring strength and mobility to ensuring psychological comfort for the patient. The collaboration between surgical teams and rehabilitation specialists is often essential to tailor recovery plans that meet individual patient needs.
Additionally, considerations such as the patient’s age, general health, and the type of surgery performed dictate the complexity and length of the rehabilitation process. Customization of these plans appears to be a significant factor affecting patient satisfaction and long-term recovery outcomes.
Immediate Postoperative Management
Immediate postoperative management focuses on monitoring and stabilizing patients in the hours and days following cervical spine surgery. During this phase, vital signs must be recorded frequently to ensure proper recovery. Monitoring for neurological changes is also essential to promptly identify possible complications.
Key tasks during this phase include:
- Observing changes in sensory and motor functions.
- Managing pain through medications prescribed by the surgical team.
- Implementing early mobilization strategies to reduce postoperative complications, like deep vein thrombosis.


A clear communication plan between healthcare providers and patients is necessary. Patients are often informed about what to expect, including potential sensations or discomfort they may experience post-surgery. They are also educated on the signs of complications so they can seek help if needed.
Long-term Rehabilitation Considerations
Long-term rehabilitation extends beyond the initial recovery phase and focuses on restoring strength, flexibility, and function. In this stage, exercise regimens may be introduced to enhance overall physical health. The aim is to reintegrate patients into their normal routine while minimizing the risk of re-injury.
Considerations for successful long-term rehabilitation include:
- Physical Therapy: Therapeutic exercises and hands-on techniques designed to improve the range of motion and strength.
- Activity Modification: Education on proper body mechanics and postural alignment to prevent future injury.
- Psychosocial Support: Mental health considerations are important, as surgery can affect psychological well-being. Support groups or counseling might be beneficial.
An organized follow-up schedule with healthcare providers is crucial. Regular assessments allow for adjustments to rehabilitation plans based on progress and evolving needs.
"The transition from surgery to rehabilitation holds significant importance in the patient's recovery journey. Detailed attention to both immediate and long-term care can alter the trajectory of healing considerably."
In summary, postoperative care and rehabilitation stand as pillars of effective cervical spine surgery outcomes. Evaluating both immediate management and long-term rehabilitation will provide a roadmap to recovery that emphasizes patient-centric strategies.
Patient Selection for Cervical Spine Surgery
Patient selection plays a crucial role in the effectiveness and safety of cervical spine surgery. The complexities of the human body and the unique nature of each patient's condition necessitate a thorough evaluation before proceeding with any surgical intervention. Tailoring the approach to fit individual needs improves surgical outcomes and reduces the risk of complications.
When considering surgical options, the clinician must assess various factors, including the patient’s medical history, the severity of symptoms, and the specific spinal disorder presented. Understanding these elements is important for making informed decisions about whether to recommend surgery.
A comprehensive assessment at this stage can determine if surgery is necessary or appropriate. Patients may present with conditions ranging from herniated discs to spinal stenosis, and the urgency of surgery can vary significantly. Surgical eligibility needs careful evaluation of neurological function, pain levels, and the impact of the disorder on daily activities.
"The goal of surgical selection is to optimize patient outcomes while minimizing risks."
This targeted approach includes both objective tests—like imaging studies—and subjective evaluations through patient-reported outcomes.
Assessing Surgical Eligibility
Assessing surgical eligibility is a detailed process. First, healthcare providers should take a thorough patient history that covers previous treatments, medication responses, and functional limitations. This history informs the likelihood of surgical benefit.
Next, physical examinations reveal crucial insights into the patient’s neurological status and pain sources. Diagnostic imaging, such as MRI or CT scans, assists in visualizing the specific pathology affecting the cervical spine. Factors like age, overall health, and comorbid conditions also influence surgical candidacy.
Patients who exhibit significant neurological deficits may have a clearer indication for surgery, while those with less severe symptoms might explore non-surgical options first. It's essential that patients understand the risks and benefits associated with surgery.
Importance of Multidisciplinary Evaluation
Involving a multidisciplinary team in the evaluation process significantly enhances patient outcomes. This team often includes neurosurgeons, orthopedic surgeons, physical therapists, and pain management specialists. Each professional contributes a unique perspective.
Such evaluations facilitate a comprehensive understanding of the patient’s condition. Collaboration helps to identify all possible treatment strategies before deciding on surgery. Additionally, this approach allows for more nuanced patient education regarding expected outcomes and recovery paths.
Moreover, multidisciplinary involvement aids in determining if adjunct therapies could be beneficial post-surgery. For example, physical therapy often plays a vital role in rehabilitation, addressing mobility and strength post-surgery. Hence, integrating these elements creates a holistic approach that ensures optimal patient care.
Future Trends in Cervical Spine Surgery
The landscape of cervical spine surgery is evolving, driven by technological advancements and improved patient care strategies. Understanding these future trends is critical for both healthcare professionals and patients. They not only influence surgical outcomes but also shape the entire patient experience. Patients may benefit from faster recovery times, less invasive procedures, and a better understanding of their conditions. Surgeons need to stay informed about these trends to apply the latest knowledge and techniques effectively.
Innovations in Surgical Techniques
Surgical techniques for cervical spine surgery are experiencing noteworthy innovations. These advancements focus on enhancing precision and reducing trauma. One significant development is the integration of robotic-assisted surgical systems. These systems provide surgeons with enhanced visualization and dexterity, leading to more precise movements and better patient outcomes.
Another area of innovation is the use of 3D printing. Surgeons can now create custom implants based on a patient's unique anatomy. This tailored approach can lead to improved fit and function of medical devices, ultimately resulting in more effective surgeries.
Some notable techniques include:
- Endoscopic spine surgery: This minimally invasive option reduces recovery times and may decrease post-operative pain.
- Navigation systems: Advanced imaging techniques allow for real-time navigation during surgery, enhancing safety and effectiveness.
Advancements in Patient Care
With an eye towards improving patient care in cervical spine surgery, several key advancements are emerging. One area of focus is the implementation of enhanced recovery after surgery (ERAS) protocols. These protocols aim to optimize recovery by minimizing the stress of surgery on the body. They include measures such as:
- Preoperative patient education
- Optimized pain management strategies
- Early mobilization post-surgery
Telemedicine also plays a growing role in patient care. Follow-up consultations can occur remotely, offering convenience and increasing access to specialists for many patients. This is particularly beneficial for those in rural areas or with mobility issues.
Advances in patient care not only enhance recovery times but also improve overall satisfaction with surgical outcomes.
End
In summary, the future trends in cervical spine surgery herald significant transformations. Innovations in surgical techniques coupled with advancements in patient care can lead to improved surgical outcomes and enhanced recovery experiences for patients. Staying abreast of these developments is essential for those involved in spinal health, ultimately allowing for the delivery of individualized and effective treatment options.







